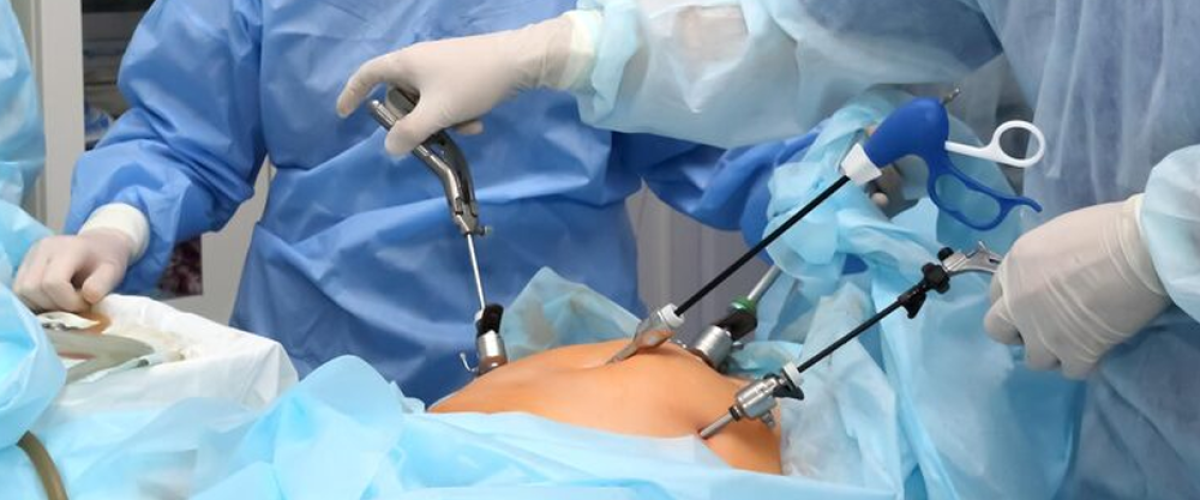
In order to relieve pain and neurological symptoms caused by herniated disc material compressing spinal nerves, endoscopic discectomy is a minimally invasive spine surgery procedure. It offers less tissue injury and a quicker recovery than a typical open discectomy.
Signs That Call for an Endoscopic Discectomy
When spinal nerves are compressed by a herniated disc (slipped or ruptured disc), it can result in:
- Sciatica is an acute, shooting pain in the legs.
- Tingling or numbness in the feet or legs.
- Weakening of the muscles (foot drop, trouble walking).
- Leg pain, but lower back pain is frequently worse.
- Rare cases of bowel or bladder dysfunction necessitate immediate surgery in cases of cauda equina syndrome.
Types of Endoscopic Discectomy
1. Percutaneous Endoscopic Lumbar Discectomy (PELD)
- Uses a tiny incision (less than 1 cm) and an endoscope with a camera.
- Best for lumbar (lower back) herniations.
2. Transforaminal Endoscopic Discectomy (TED)
- Accesses the disc through the foramen (natural nerve opening).
- Minimizes muscle/tissue damage.
3. Posterior Endoscopic Discectomy
- Used for central or severe herniations.